Search
- Page Path
- HOME > Search
- Diabetes, obesity and metabolism
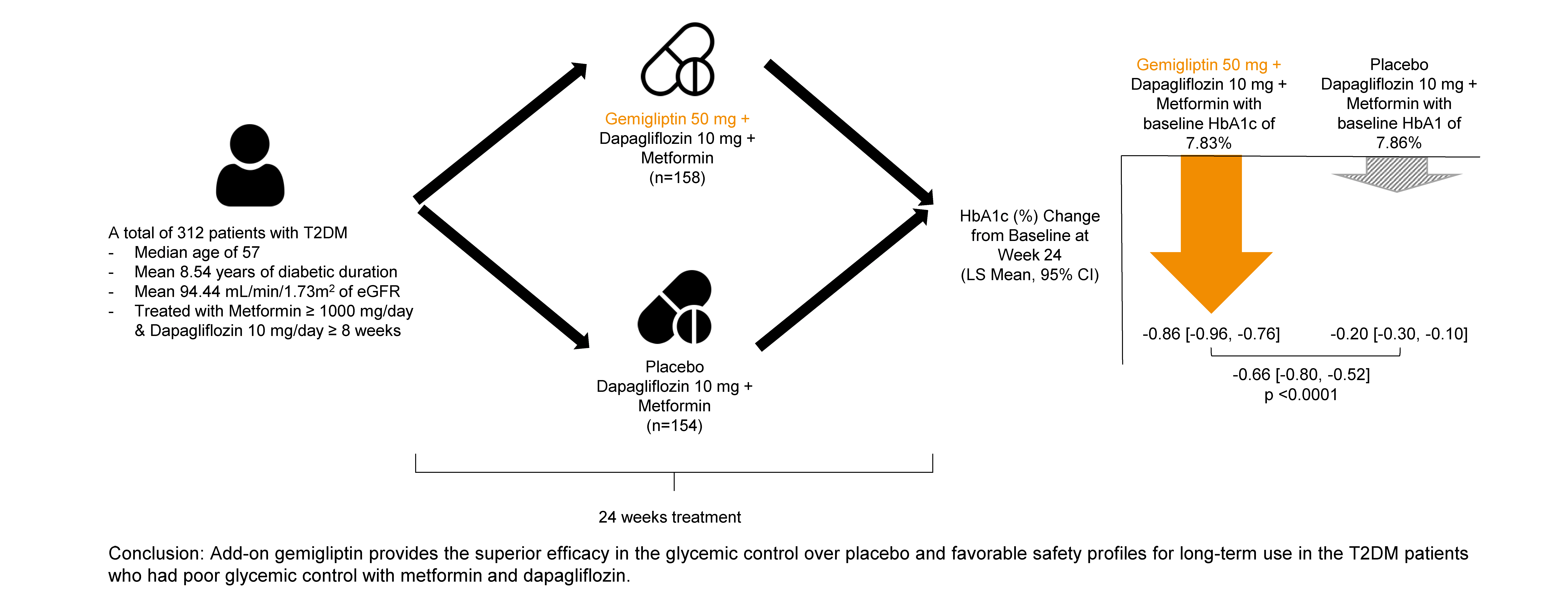
- Efficacy of Gemigliptin Add-on to Dapagliflozin and Metformin in Type 2 Diabetes Patients: A Randomized, Double-Blind, Placebo-Controlled Study (SOLUTION)
- Byung Wan Lee, KyungWan Min, Eun-Gyoung Hong, Bon Jeong Ku, Jun Goo Kang, Suk Chon, Won-Young Lee, Mi Kyoung Park, Jae Hyeon Kim, Sang Yong Kim, Keeho Song, Soon Jib Yoo
- Endocrinol Metab. 2023;38(3):328-337. Published online June 28, 2023
- DOI: https://doi.org/10.3803/EnM.2023.1688
- 2,406 View
- 262 Download
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material PubReader
PubReader  ePub
ePub - Background
This study evaluated the efficacy and safety of add-on gemigliptin in patients with type 2 diabetes mellitus (T2DM) who had inadequate glycemic control with metformin and dapagliflozin.
Methods
In this randomized, placebo-controlled, parallel-group, double-blind, phase III study, 315 patients were randomized to receive either gemigliptin 50 mg (n=159) or placebo (n=156) with metformin and dapagliflozin for 24 weeks. After the 24-week treatment, patients who received the placebo were switched to gemigliptin, and all patients were treated with gemigliptin for an additional 28 weeks.
Results
The baseline characteristics were similar between the two groups, except for body mass index. At week 24, the least squares mean difference (standard error) in hemoglobin A1c (HbA1c) changes was –0.66% (0.07) with a 95% confidence interval of –0.80% to –0.52%, demonstrating superior HbA1c reduction in the gemigliptin group. After week 24, the HbA1c level significantly decreased in the placebo group as gemigliptin was administered, whereas the efficacy of HbA1c reduction was maintained up to week 52 in the gemigliptin group. The safety profiles were similar: the incidence rates of treatment-emergent adverse events up to week 24 were 27.67% and 29.22% in the gemigliptin and placebo groups, respectively. The safety profiles after week 24 were similar to those up to week 24 in both groups, and no new safety findings, including hypoglycemia, were noted.
Conclusion
Add-on gemigliptin was well tolerated, providing comparable safety profiles and superior efficacy in glycemic control over placebo for long-term use in patients with T2DM who had poor glycemic control with metformin and dapagliflozin.

- Glucocorticoid-Induced Diabetes Mellitus: An Important but Overlooked Problem
- Sunghwan Suh, Mi Kyoung Park
- Endocrinol Metab. 2017;32(2):180-189. Published online May 29, 2017
- DOI: https://doi.org/10.3803/EnM.2017.32.2.180
- 15,232 View
- 589 Download
- 108 Web of Science
- 117 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader  ePub
ePub Glucocorticoids are widely used as potent anti-inflammatory and immunosuppressive drugs to treat a wide range of diseases. However, they are also associated with a number of side effects, including new-onset hyperglycemia in patients without a history of diabetes mellitus (DM) or severely uncontrolled hyperglycemia in patients with known DM. Glucocorticoid-induced diabetes mellitus (GIDM) is a common and potentially harmful problem in clinical practice, affecting almost all medical specialties, but is often difficult to detect in clinical settings. However, scientific evidence is lacking regarding the effects of GIDM, as well as strategies for prevention and treatment. Similarly to nonsteroid-related DM, the principles of early detection and risk factor modification apply. Screening for GIDM should be considered in all patients treated with medium to high doses of glucocorticoids. Challenges in the management of GIDM stem from wide fluctuations in postprandial hyperglycemia and the lack of clearly defined treatment protocols. Together with lifestyle measures, hypoglycemic drugs with insulin-sensitizing effects are indicated. However, insulin therapy is often unavoidable, to the point that insulin can be considered the drug of choice. The treatment of GIDM should take into account the degree and pattern of hyperglycemia, as well as the type, dose, and schedule of glucocorticoid used. Moreover, it is essential to instruct the patient and/or the patient's family about how to perform the necessary adjustments. Prospective studies are needed to answer the remaining questions regarding GIDM.
-
Citations
Citations to this article as recorded by- COVID‐19 associated mucormycosis surge: A review on multi‐pathway mechanisms
Mohsen Pourazizi, Atousa Hakamifard, Alireza Peyman, Rasoul Mohammadi, Shakiba Dehghani, Najmeh Tavousi, Nastaran‐Sadat Hosseini, Hamed Azhdari Tehrani, Bahareh Abtahi‐Naeini
Parasite Immunology.2024;[Epub] CrossRef - Drug-induced hyperglycemia and diabetes
Marie-Anne Heurtebize, Jean-Luc Faillie
Therapies.2024; 79(2): 221. CrossRef - Immunosuppression in solid organ–transplant recipients and impact on nutrition support
Nicole K. Wilson, Ann D. Kataria
Nutrition in Clinical Practice.2024; 39(1): 109. CrossRef - The effect of different types of oral or intravenous corticosteroids on capillary blood glucose levels in hospitalized inpatients with and without diabetes
Vaishali Limbachia, Ian Nunney, Daniel J. Page, Hannah A. Barton, Leena K. Patel, Georgia N. Thomason, Stephan L. Green, Kieran F.J. Lewis, Ketan Dhatariya
Clinical Therapeutics.2024; 46(2): e59. CrossRef - Incidence and Characteristics of the Hyperosmolar Hyperglycemic State: A Danish Cohort Study
Emilie V. Rosager, Amalia Lærke K. Heltø, Cathrine U. Fox Maule, Lennart Friis-Hansen, Janne Petersen, Finn E. Nielsen, Steen B. Haugaard, Rasmus Gregersen
Diabetes Care.2024; 47(2): 272. CrossRef - Cortisol levels across the lifespan in common marmosets (Callithrix jacchus)
Matthew Lopez, Amaya Seidl, Kimberley A. Phillips
American Journal of Primatology.2024;[Epub] CrossRef - Belimumab in a Patient with Systemic Lupus Erythematosus with Juvenile Onset and Steroid-induced Diabetes: Clinical Case
Maria I. Kaleda, Irina P. Nikishina, Alesya V. Firsa
Current Pediatrics.2024; 22(6): 546. CrossRef - Optimal initial insulin dosage for managing steroid-induced hyperglycemia in hospitalized COVID-19 patients: A retrospective single-center study
Nuttavadee Ketaroonrut, Sasisopin Kiertiburanakul, Chutintorn Sriphrapradang
SAGE Open Medicine.2024;[Epub] CrossRef - Important aspects of carbohydrate metabolism disorders development in hematology/oncology patients during therapy with glucocorticosteroids: a review of the literature
N. T. Vatutin, E. V. Sklyannaya, V. V. Gribov
Oncohematology.2024; 19(2): 118. CrossRef - The safety and use of perioperative dexamethasone in the perioperative management of primary sporadic supratentorial meningiomas
Felix Arlt, Alim Emre Basaran, Markus Vogel, Martin Vychopen, Clemens Seidel, Alonso Barrantes-Freer, Erdem Güresir, Johannes Wach
Frontiers in Oncology.2024;[Epub] CrossRef - Sars-Cov2 Induced Biochemical Mechanisms in Liver Damage and Intestinal Lesions
Liudmila V. Spirina, Vladimir N. Masunov, Denis A. Dyakov, Olga E. Akbasheva, Amina Y. Kebekbayeva, Igor Yu. Shuvalov, Nadezhda V. Masunova, Irina V. Kovaleva, Yumzhana Dagbaeva
Indian Journal of Clinical Biochemistry.2023; 38(4): 437. CrossRef - Mouse Pancreatic Peptide Hormones Probed at the Sub-Single-Islet Level: The Effects of Acute Corticosterone Treatment
Aleksandra Antevska, Connor C. Long, Samuel D. Dupuy, J. Jason Collier, Michael D. Karlstad, Thanh D. Do
Journal of Proteome Research.2023; 22(1): 235. CrossRef - Type 1 and other types of diabetes mellitus in the perioperative period. What the anaesthetist should know
Robert van Wilpe, Abraham H. Hulst, Sarah.E. Siegelaar, J. Hans DeVries, Benedikt Preckel, Jeroen Hermanides
Journal of Clinical Anesthesia.2023; 84: 111012. CrossRef - Continuous Glucose Monitoring of Steroid-Induced Hyperglycemia in Patients With Dermatologic Diseases
Monika Kleinhans, Lea Jessica Albrecht, Sven Benson, Dagmar Fuhrer, Joachim Dissemond, Susanne Tan
Journal of Diabetes Science and Technology.2023; : 193229682211479. CrossRef - The Effects of Daily Prednisone and Tocilizumab on Hemoglobin A1c During the Treatment of Giant Cell Arteritis
Naomi J. Patel, Veronica Tozzo, John M. Higgins, John H. Stone
Arthritis & Rheumatology.2023; 75(4): 586. CrossRef - Characterization, evolution and risk factors of diabetes and prediabetes in a pediatric cohort of renal and liver transplant recipients
Sophie Welsch, Virginie Mailleux, Priscilla le Hardy de Beaulieu, Nadejda Ranguelov, Nathalie Godefroid, Annie Robert, Xavier Stephenne, Isabelle Scheers, Raymond Reding, Etienne M. Sokal, Philippe A. Lysy
Frontiers in Pediatrics.2023;[Epub] CrossRef - The safety of perioperative dexamethasone with antiemetic dosage in surgical patients with diabetes mellitus: a systematic review and meta-analysis
Qian-Yun Pang, Jing-Yun Wang, Xiao-Long Liang, Yan Jiang, Hong-Liang Liu
Perioperative Medicine.2023;[Epub] CrossRef - Link between Blood Cell-Associated Inflammatory Indices and Chemotherapy-Induced Hyperglycemia in Women Affected with Breast Cancer: Clinical Studies
Krishna Prasad, Suresh Rao, Sanath Kumar Hegde, Thomas George, Rhea Katherine D'souza, Sucharitha Suresh, Manjeshwar Shrinath Baliga
South Asian Journal of Cancer.2023; 12(02): 118. CrossRef - Hyperglycemia and Glycemic Variability Associated with Glucocorticoids in Women without Pre-Existing Diabetes Undergoing Neoadjuvant or Adjuvant Taxane Chemotherapy for Early-Stage Breast Cancer
Dana Mahin, Sayeh Moazami Lavasani, Leon Cristobal, Niki Tank Patel, Mina Sedrak, Daphne Stewart, James Waisman, Yuan Yuan, Wai Yu, Raynald Samoa, Nora Ruel, Susan E. Yost, Hayley Lee, Sung Hee Kil, Joanne E. Mortimer
Journal of Clinical Medicine.2023; 12(5): 1906. CrossRef - Oral mometasone furoate administration preserves anti-inflammatory action with fewer metabolic adverse effects in rats
Priscila L. Zimath, Milena S. Almeida, Maciel A. Bruxel, Alex Rafacho
Biochemical Pharmacology.2023; 210: 115486. CrossRef - Regeneration of an infected skin wound under conditions of experimental steroid hyperglycemia
L. A. Balykova, V. I. Inchina, T. V. Tarasova, D. A. Khaydar, L. M. Mosina, I. V. Saushev, A. V. Kuchuk, A. Mutvakel, I. V. Begoulov, R. S. Tarasov, P. V. Ageev, D. S. Ovchenkov
Research and Practical Medicine Journal.2023; 10(1): 90. CrossRef - Time to reposition sulfonylureas in type 2 diabetes management in Indian context: A pragmatic practical approach
Ashok Kumar Das, Banshi Saboo, Rajeev Chawla, S. R. Aravind, Rajesh Rajput, Awadhesh K. Singh, J. J. Mukherjee, Ashok Jhingan, Parag Shah, Vaishali Deshmukh, Shailaja Kale, Shalini Jaggi, G. R. Sridhar, Rajnish Dhediya, Kumar Gaurav
International Journal of Diabetes in Developing Countries.2023; 43(6): 856. CrossRef - Risk for Newly Diagnosed Type 2 Diabetes Mellitus after COVID-19 among Korean Adults: A Nationwide Matched Cohort Study
Jong Han Choi, Kyoung Min Kim, Keeho Song, Gi Hyeon Seo
Endocrinology and Metabolism.2023; 38(2): 245. CrossRef - Zein nanoparticles as oral carrier for mometasone furoate delivery
Priscila Zimath, Soraia Pinto, Sofia Dias, Alex Rafacho, Bruno Sarmento
Drug Delivery and Translational Research.2023; 13(11): 2948. CrossRef - Impact of Diabetes in COVID-19 Associated Mucormycosis and its Management:
A Non-Systematic Literature Review
Muhammed Rashid, Asha K. Rajan, Girish Thunga, Vishal Shanbhag, Sreedharan Nair
Current Diabetes Reviews.2023;[Epub] CrossRef - Adrenomedullin peptides and precursor levels in relation to haemodynamics and prognosis after heart transplantation
Abdulla Ahmed, Kriss Kania, Hebba Abdul Rahim, Salaheldin Ahmed, Göran Rådegran
ESC Heart Failure.2023; 10(4): 2427. CrossRef - Part II: Interactive case: Drug‐induced endocrine disorders
Amy C. Donihi
JACCP: JOURNAL OF THE AMERICAN COLLEGE OF CLINICAL PHARMACY.2023; 6(6): 663. CrossRef - Treating the Side Effects of Exogenous Glucocorticoids; Can We Separate the Good From the Bad?
Riccardo Pofi, Giorgio Caratti, David W Ray, Jeremy W Tomlinson
Endocrine Reviews.2023; 44(6): 975. CrossRef - Disease-modifying anti-rheumatic drugs associated with different diabetes risks in patients with rheumatoid arthritis
Yu-Jih Su, Hui-Ming Chen, Tien-Ming Chan, Tien-Tsai Cheng, Shan-Fu Yu, Jia-Feng Chen, Chun-Yu Lin, Chung-Yuan Hsu
RMD Open.2023; 9(3): e003045. CrossRef - The Prevalence of Diabetes Mellitus Type II (DMII) in the Multiple Sclerosis Population: A Systematic Review and Meta-Analysis
Vasileios Giannopapas, Lina Palaiodimou, Dimitrios Kitsos, Georgia Papagiannopoulou, Konstantina Stavrogianni, Athanasios Chasiotis, Maria Kosmidou, John S. Tzartos, George P. Paraskevas, Daphne Bakalidou, Georgios Tsivgoulis, Sotirios Giannopoulos
Journal of Clinical Medicine.2023; 12(15): 4948. CrossRef - Diabetes Mellitus Secondary to Endocrine Diseases: An Update of Diagnostic and Treatment Particularities
Mihaela Simona Popoviciu, Lorena Paduraru, Raluca Marinela Nutas, Alexandra Maria Ujoc, Galal Yahya, Kamel Metwally, Simona Cavalu
International Journal of Molecular Sciences.2023; 24(16): 12676. CrossRef - Usefulness of Indian Diabetes Risk Score in Predicting Treatment-Induced Hyperglycemia in Women Undergoing Adjuvant Chemotherapy for Breast Cancer
Krishna Prasad, Sanath Hegde, Suresh Rao, Rhea Katherine D'souza, Thomas George, Manjeshwar Shrinath Baliga, Sucharitha Suresh
South Asian Journal of Cancer.2023;[Epub] CrossRef - The inverse association between DNA gaps and HbA1c levels in type 2 diabetes mellitus
Jirapan Thongsroy, Apiwat Mutirangura
Scientific Reports.2023;[Epub] CrossRef - Corticosteroids for COVID-19: worth it or not?
Fariya Akter, Yusha Araf, Mohammad Jakir Hosen
Molecular Biology Reports.2022; 49(1): 567. CrossRef - Evidence-Based Management of Steroid-Induced Hyperglycemia in the Inpatient Setting
Lauren Longaker, Jennifer N. Clements
ADCES in Practice.2022; 10(1): 40. CrossRef - Is Methylprednisolone Acetate-Related Insulin Resistance Preventable in Cats?
Karine Marchioro Leal, Mariana Barcelos Rocha, Fernanda Venzon Varela, Luana Rodrigues, Priscila Viau Furtado, Fernanda Vieira Amorim da Costa, Álan Gomes Pöppl
Topics in Companion Animal Medicine.2022; 49: 100648. CrossRef - Ac3IV, a V1a and V1b receptor selective vasopressin analogue, protects against hydrocortisone-induced changes in pancreatic islet cell lineage
Shruti Mohan, Ryan A. Lafferty, Peter R. Flatt, R. Charlotte Moffett, Nigel Irwin
Peptides.2022; 152: 170772. CrossRef - Hospital management of hyperglycemia in the context of COVID-19: evidence-based clinical considerations
Thiago Bosco Mendes, Alexandre Barbosa Câmara-de-Souza, Bruno Halpern
Diabetology & Metabolic Syndrome.2022;[Epub] CrossRef - When therapeutic drugs lead to diabetes
Bruno Fève, André J. Scheen
Diabetologia.2022; 65(5): 751. CrossRef - Nutrition implications of intrinsic restrictive lung disease
Sylvia Rinaldi, Christine Balsillie, Cassandra Truchon, Awatif AL‐Mubarak, Marco Mura, Janet Madill
Nutrition in Clinical Practice.2022; 37(2): 239. CrossRef - Coinfection by Aspergillus and Mucoraceae Species in Two Cases of Acute Rhinosinusitis as a Complication of COVID-19
Payam Tabarsi, Somayeh Sharifynia, Mihan Pourabdollah Toutkaboni, Zahra Abtahian, Mohammad Rahdar, Arefeh Sadat Mirahmadian, Atousa Hakamifard, Simone Cesaro
Case Reports in Medicine.2022; 2022: 1. CrossRef - Case Report: Neratinib Therapy Improves Glycemic Control in a Patient With Type 2 Diabetes and Breast Cancer
Vasileios Angelis, Stephen R. D. Johnston, Amin Ardestani, Kathrin Maedler
Frontiers in Endocrinology.2022;[Epub] CrossRef - The Impact of Deranged Glucose Metabolism and Diabetes in the Pathogenesis
and Prognosis of the Novel SARS-CoV-2: A Systematic Review of Literature
Victor O. Ukwenya, Sunday A. Adelakun, Temiloluwa A. Fuwape, Ayotunde S. Adeagbo
Current Diabetes Reviews.2022;[Epub] CrossRef - Could anakinra outmatch dexamethasone/tocilizumab in COVID-19?
Rahul Gupta
Bulletin of the National Research Centre.2022;[Epub] CrossRef - Circadian clock, diurnal glucose metabolic rhythm, and dawn phenomenon
Fei Peng, Xin Li, Fang Xiao, Ruxing Zhao, Zheng Sun
Trends in Neurosciences.2022; 45(6): 471. CrossRef - 3,3′,4,5′-Tetramethoxy-trans-stilbene Improves Insulin Resistance by Activating the IRS/PI3K/Akt Pathway and Inhibiting Oxidative Stress
Yi Tan, Lingchao Miao, Jianbo Xiao, Wai San Cheang
Current Issues in Molecular Biology.2022; 44(5): 2175. CrossRef - Management of Glucocorticoid-Induced Hyperglycemia
Parag Shah, Sanjay Kalra, Yogesh Yadav, Nilakshi Deka, Tejal Lathia, Jubbin Jagan Jacob, Sunil Kumar Kota, Saptarshi Bhattacharya, Sharvil S Gadve, KAV Subramanium, Joe George, Vageesh Iyer, Sujit Chandratreya, Pankaj Kumar Aggrawal, Shailendra Kumar Sing
Diabetes, Metabolic Syndrome and Obesity: Targets and Therapy.2022; Volume 15: 1577. CrossRef - Effects of glucocorticoids on interstitial glucose concentrations in individuals with hematologic cancer and without known diagnosis of diabetes: a pilot study
Marcos Tadashi Kakitani Toyoshima, Priscilla Cukier, Alexandre Barbosa Câmara de Souza, Juliana Pereira, Ana Oliveira Hoff, Marcia Nery
einstein (São Paulo).2022;[Epub] CrossRef - Mucormycosis in the COVID-19 Environment: A Multifaceted Complication
Rohit Sharma, Praveen Kumar, Abdur Rauf, Ashun Chaudhary, Pradeep Kumar Prajapati, Talha Bin Emran, Clara Mariana Gonçalves Lima, Carlos Adam Conte-Junior
Frontiers in Cellular and Infection Microbiology.2022;[Epub] CrossRef - Black pepper oil (Piper nigrum L.) mitigates dexamethasone induced pancreatic damage via modulation of oxidative and nitrosative stress
Mona F. Mahmoud, Asmaa M. Elmaghraby, Noura Ali, Islam Mostafa, Assem M. El-Shazly, Mohamed A.O. Abdelfattah, Mansour Sobeh
Biomedicine & Pharmacotherapy.2022; 153: 113456. CrossRef - Various Coated Barrier Membranes for Better Guided Bone Regeneration: A Review
Ji-Youn Kim, Jun-Beom Park
Coatings.2022; 12(8): 1059. CrossRef - RETROSPECTIVE STUDY ON GLYCAEMIC CONTROL OF THE MIDDLE-AGED PATIENTS RECEIVING STEROID THERAPY IN COVID ICU
Sayantan Dutta, Sumanta Ghosh Maulik, Jisnu Nayak
PARIPEX INDIAN JOURNAL OF RESEARCH.2022; : 1. CrossRef - Risk of diabetes and the impact on preexisting diabetes in patients with lymphoma treated with steroid-containing immunochemotherapy
Joachim Baech, Marianne Tang Severinsen, Andreas K. Øvlisen, Henrik Frederiksen, Peter Vestergaard, Christian Torp-Pedersen, Judit Jørgensen, Michael Roost Clausen, Christian B. Poulsen, Peter Brown, Anne Ortved Gang, Robert Schou Pedersen, Karin Ekström
Blood Advances.2022; 6(15): 4427. CrossRef - Diabètes pharmaco-induits : quatre classes médicamenteuses au cœur de notre pratique clinique
André J. Scheen, Bruno Fève
Médecine des Maladies Métaboliques.2022; 16(7): 627. CrossRef - Dexamethasone-induced derangement in some liver function parameters: Hepatoprotective effect of L-Citrulline
Timothy Danboyi, Abdulazeez Jimoh, Evelyn Hassan-Danboyi, AbdulWahab Alhassan, AugustineBanlibo Dubo
Nigerian Journal of Experimental and Clinical Biosciences.2022; 10(3): 74. CrossRef - Polypharmacy Patterns in Multimorbid Older People with Cardiovascular Disease: Longitudinal Study
Noemí Villén, Albert Roso-Llorach, Carlos Gallego-Moll, Marc Danes-Castells, Sergio Fernández-Bertolin, Amelia Troncoso-Mariño, Monica Monteagudo, Ester Amado, Concepción Violán
Geriatrics.2022; 7(6): 141. CrossRef - Increased risk of type 2 diabetes in patients with systemic lupus erythematosus: A nationwide cohort study in Taiwan
Yeong-Jang Lin, Chih-Chiang Chien, Chung-Han Ho, Hung-An Chen, Chao-Yu Chen
Medicine.2022; 101(51): e32520. CrossRef - Synthetic Pharmacotherapy for Systemic Lupus Erythematosus: Potential Mechanisms of Action, Efficacy, and Safety
Angélica María Téllez Arévalo, Abraham Quaye, Luis Carlos Rojas-Rodríguez, Brian D. Poole, Daniela Baracaldo-Santamaría, Claudia M. Tellez Freitas
Medicina.2022; 59(1): 56. CrossRef - Effect of Ficus lacor Buch. Ham. Fruit Extract on Dexamethasone Induced Insulin Resistant Rats
V. S. Mule, N. S. Naikwade
Research Journal of Pharmacy and Technology.2022; : 5559. CrossRef - Prednisolone-induced diabetes mellitus in the cat: a historical cohort
Sivert Nerhagen, Hanne L Moberg, Gudrun S Boge, Barbara Glanemann
Journal of Feline Medicine and Surgery.2021; 23(2): 175. CrossRef - Mechanisms and Clinical Applications of Glucocorticoid Steroids in Muscular Dystrophy
Mattia Quattrocelli, Aaron S. Zelikovich, Isabella M. Salamone, Julie A. Fischer, Elizabeth M. McNally
Journal of Neuromuscular Diseases.2021; 8(1): 39. CrossRef - A practical approach to the clinical challenges in initiation of basal insulin therapy in people with type 2 diabetes
Thomas Forst, Pratik Choudhary, Doron Schneider, Bruno Linetzky, Paolo Pozzilli
Diabetes/Metabolism Research and Reviews.2021;[Epub] CrossRef - Incidence and control of steroid-induced hyperglycaemia in hospitalised patients at a tertiary care centre for lung diseases
Matej Dobravc Verbič, Jasna Gruban, Mojca Kerec Kos
Pharmacological Reports.2021; 73(3): 796. CrossRef - Epigenetics in blood–brain barrier disruption
Stephanie A. Ihezie, Iny Elizebeth Mathew, Devin W. McBride, Ari Dienel, Spiros L. Blackburn, Peeyush Kumar Thankamani Pandit
Fluids and Barriers of the CNS.2021;[Epub] CrossRef - Risk factors for corticosteroid-induced hyperglycemia requiring insulin therapy in hospitalized patients without diabetes
Catherine Li, Patricia Krause, Gretchen Stern
Endocrine.2021; 73(2): 476. CrossRef - Population pharmacodynamic modeling of intramuscular and oral dexamethasone and betamethasone effects on six biomarkers with circadian complexities in Indian women
Wojciech Krzyzanski, Mark A. Milad, Alan H. Jobe, Thomas Peppard, Robert R. Bies, William J. Jusko
Journal of Pharmacokinetics and Pharmacodynamics.2021; 48(3): 411. CrossRef - Hormonal activity in commonly used Black hair care products: evaluating hormone disruption as a plausible contribution to health disparities
Tamarra James-Todd, Lisa Connolly, Emma V. Preston, Marlee R. Quinn, Monika Plotan, Yuling Xie, Bharathi Gandi, Shruthi Mahalingaiah
Journal of Exposure Science & Environmental Epidemiology.2021; 31(3): 476. CrossRef - New‐onset diabetes in “long COVID”
Thirunavukkarasu Sathish, Mary Chandrika Anton, Tharsan Sivakumar
Journal of Diabetes.2021; 13(8): 693. CrossRef - Glucocorticoid-Induced Exacerbation of Mycobacterial Infection Is Associated With a Reduced Phagocytic Capacity of Macrophages
Yufei Xie, Jiajun Xie, Annemarie H. Meijer, Marcel J. M. Schaaf
Frontiers in Immunology.2021;[Epub] CrossRef - Glucocorticoid signaling in pancreatic islets modulates gene regulatory programs and genetic risk of type 2 diabetes
Anthony Aylward, Mei-Lin Okino, Paola Benaglio, Joshua Chiou, Elisha Beebe, Jose Andres Padilla, Sharlene Diep, Kyle J. Gaulton, Michael L. Stitzel
PLOS Genetics.2021; 17(5): e1009531. CrossRef - A Practical Guide for the Management of Steroid Induced Hyperglycaemia in the Hospital
Felix Aberer, Daniel A. Hochfellner, Harald Sourij, Julia K. Mader
Journal of Clinical Medicine.2021; 10(10): 2154. CrossRef - Combination of Bawang Dayak Extract and Acarbose against Male White Rat Glucose Levels
Aditya Maulana Perdana Putra, Ratih Pratiwi Sari, Siska Musiam
Borneo Journal of Pharmacy.2021; 4(2): 84. CrossRef - Role of Gliclazide in safely navigating type 2 diabetes mellitus patients towards euglycemia: Expert opinion from India
Subhash Wangnoo, M. Shunmugavelu, Sagili Vijaya Bhaskar Reddy, Vijay Negalur, Shreerang Godbole, Vinay K Dhandhania, Nareen Krishna, Kumar Gaurav
Endocrine and Metabolic Science.2021; 4: 100102. CrossRef - Genome-Wide Differential Methylation Profiles from Two Terpene-Rich Medicinal Plant Extracts Administered in Osteoarthritis Rats
Younhee Shin, Sathiyamoorthy Subramaniyam, Jin-Mi Chun, Ji-Hyeon Jeon, Ji-Man Hong, Hojin Jung, Boseok Seong, Chul Kim
Plants.2021; 10(6): 1132. CrossRef - Chronic glucocorticoid treatment induces hepatic lipid accumulation and hyperinsulinaemia in part through actions on AgRP neurons
Erika Harno, Charlotte Sefton, Jonathan R. Wray, Tiffany-Jayne Allen, Alison Davies, Anthony P. Coll, Anne White
Scientific Reports.2021;[Epub] CrossRef - Endocrine Disorders in Autoimmune Rheumatological Diseases: A Focus on Thyroid Autoimmune Diseases and on the Effects of Chronic Glucocorticoid Treatment
Filippo Egalini, Mirko Parasiliti Caprino, Giulia Gaggero, Vincenzo Cappiello, Jacopo Giannelli, Ruth Rossetto Giaccherino, Loredana Pagano, Roberta Giordano
Endocrines.2021; 2(3): 171. CrossRef - Current cancer therapies and their influence on glucose control
Carly Yim, Kerry Mansell, Nassrein Hussein, Terra Arnason
World Journal of Diabetes.2021; 12(7): 1010. CrossRef - Immune‐checkpoint inhibitor‐associated diabetes compared to other diabetes types ‐ A prospective, matched control study
Sascha R. Tittel, Katharina Laubner, Sebastian M. Schmid, Stefan Kress, Sigrun Merger, Wolfram Karges, Frank J. Wosch, Marcus Altmeier, Marianne Pavel, Reinhard W. Holl
Journal of Diabetes.2021; 13(12): 1007. CrossRef - Connecting the Dots: Interplay of Pathogenic Mechanisms between COVID-19 Disease and Mucormycosis
Hariprasath Prakash, Anna Skiada, Raees Ahmad Paul, Arunaloke Chakrabarti, Shivaprakash Mandya Rudramurthy
Journal of Fungi.2021; 7(8): 616. CrossRef - Antioxidant effects of L-citrulline supplementation in high-fat diet- and dexamethasone-induced Type-2 diabetes mellitus in wistar rats (Rattus norvegicus)
Evelyn Hassan-Danboyi, Abdulazeez Jimoh, Abdulwahab Alhassan, Timothy Danboyi, KabirAhmed Mohammed, AugustineBanlibo Dubo, Jamilu Haruna, BulusBilly Yakubu
Nigerian Journal of Experimental and Clinical Biosciences.2021; 9(2): 95. CrossRef - ASSESSMENT OF THE POSSIBLE CAUSES OF DIABETES MELLITUS DEVELOPED IN PATIENTS POST COVID-19 TREATMENT IN A TERTIARY CARE HOSPITAL
KHUJITH RAJUENI, RUTUJA AMBEKAR, HITENDRAPAL SOLANKI, ABDULRAHAMAN ABUBAKAR MOMIN, SUNITA PAWAR
International Journal of Pharmacy and Pharmaceutical Sciences.2021; : 11. CrossRef - Potent Anti-Inflammatory, Arylpyrazole-Based Glucocorticoid Receptor Agonists That Do Not Impair Insulin Secretion
Brandon J. Kennedy, Ashley M. Lato, Alexander R. Fisch, Susan J. Burke, Justin K. Kirkland, Carson W. Prevatte, Lee E. Dunlap, Russell T. Smith, Konstantinos D. Vogiatzis, J. Jason Collier, Shawn R. Campagna
ACS Medicinal Chemistry Letters.2021; 12(10): 1568. CrossRef - Diabetes in COVID-19 patients: challenges and possible management strategies
Riyan Al Islam Reshad, Sumaiya Hafiz Riana, Mohammad Al-baruni Chowdhury, Abu Tayab Moin, Faruque Miah, Bishajit Sarkar, Nurnabi Azad Jewel
The Egyptian Journal of Bronchology.2021;[Epub] CrossRef - Excess Body Mass—A Factor Leading to the Deterioration of COVID-19 and Its Complications—A Narrative Review
Weronika Gryczyńska, Nikita Litvinov, Bezawit Bitew, Zuzanna Bartosz, Weronika Kośmider, Paweł Bogdański, Damian Skrypnik
Viruses.2021; 13(12): 2427. CrossRef - Risk of Future Type 2 Diabetes Mellitus in Patients Developing Steroid-Induced Hyperglycemia During Hospitalization for Chronic Obstructive Pulmonary Disease Exacerbation
Jagriti Upadhyay, Nitin Trivedi, Amos Lal
Lung.2020; 198(3): 525. CrossRef - Acetylation of Hsp90 reverses dexamethasone-mediated inhibition of insulin secretion
Kecheng Zhu, Yumei Zhang, Juan Zhang, Feiye Zhou, Linlin Zhang, Shushu Wang, Qin Zhu, Qianqian Liu, Xiao Wang, Libin Zhou
Toxicology Letters.2020; 320: 19. CrossRef - Use of inhaled corticosteroids and the risk of developing type 2 diabetes in patients with chronic obstructive pulmonary disease
Mohamad Isam Saeed, Josefin Eklöf, Imane Achir, Pradeesh Sivapalan, Howraman Meteran, Anders Løkke, Tor Biering‐Sørensen, Filip Krag Knop, Jens‐Ulrik Stæhr Jensen
Diabetes, Obesity and Metabolism.2020; 22(8): 1348. CrossRef Patterns of Glucose Fluctuation are Challenging in Patients Treated for Non-Hodgkin’s Lymphoma
Andreja Marić, Tanja Miličević, Jelena Vučak Lončar, Davor Galušić, Maja Radman
International Journal of General Medicine.2020; Volume 13: 131. CrossRef- Metformin's effectiveness in preventing prednisone-induced hyperglycemia in hematological cancers
Lucy A Ochola, David G Nyamu, Eric M Guantai, Irene W Weru
Journal of Oncology Pharmacy Practice.2020; 26(4): 823. CrossRef - Study rationale and design of the EANITIATE study (EmpAgliflozin compared to NPH Insulin for sTeroId diAbeTEs) - a randomized, controlled, multicenter trial of safety and efficacy of treatment with empagliflozin compared with NPH-insulin in patients with
Carina Kirstine Klarskov, Helga Holm Schultz, Frederik Persson, Tomas Møller Christensen, Thomas Peter Almdal, Ole Snorgaard, Katrine Bagge Hansen, Ulrik Pedersen-Bjergaard, Peter Lommer Kristensen
BMC Endocrine Disorders.2020;[Epub] CrossRef - Implementation of a Weight-Based Protocol for the Management of Steroid-Induced Hyperglycemia
Alyson K. Myers, Mahmuda Khan, Sebastian Choi, Patricia Garnica, Guillaume Stoffels, Amanda Lin
American Journal of Therapeutics.2020; 27(4): e392. CrossRef - The difference between steroid diabetes mellitus and type 2 diabetes mellitus: a whole-body 18F-FDG PET/CT study
Qingqing Zhao, Jinxin Zhou, Yu Pan, Huijun Ju, Liying Zhu, Yang Liu, Yifan Zhang
Acta Diabetologica.2020; 57(11): 1383. CrossRef - Glucocorticoid dose-dependent risk of type 2 diabetes in six immune-mediated inflammatory diseases: a population-based cohort analysis
Jianhua Wu, Sarah L Mackie, Mar Pujades-Rodriguez
BMJ Open Diabetes Research & Care.2020; 8(1): e001220. CrossRef - Diabète et corticoïdes : nouveautés et aspects pratiques
M. Bastin, F. Andreelli
La Revue de Médecine Interne.2020; 41(9): 607. CrossRef - Dexamethasone in the era of COVID-19: friend or foe? An essay on the effects of dexamethasone and the potential risks of its inadvertent use in patients with diabetes
Janine Alessi, Giovana B. de Oliveira, Beatriz D. Schaan, Gabriela H. Telo
Diabetology & Metabolic Syndrome.2020;[Epub] CrossRef - Glycemic Response to Oral Dexamethasone Predicts Incident Prediabetes in Normoglycemic Subjects With Parental Diabetes
Ebenezer Nyenwe, Deirdre James, Jim Wan, Sam Dagogo-Jack
Journal of the Endocrine Society.2020;[Epub] CrossRef - Outcomes of Hospitalized Patients with Glucocorticoid-Induced Hyperglycemia—A Retrospective Analysis
Neele Delfs, Tristan Struja, Sandra Gafner, Thaddaeus Muri, Ciril Baechli, Philipp Schuetz, Beat Mueller, Claudine Angela Blum
Journal of Clinical Medicine.2020; 9(12): 4079. CrossRef - Incidence of Hyperglycemia/Secondary Diabetes in Women who have Undergone Curative Chemotherapy for Breast Cancer: First Study from India
Suresh Rao, Krishna Prasad, Soniya Abraham, Thomas George, Supreeth Kakkaje Chandran, Manjeshwar Shrinath Baliga
South Asian Journal of Cancer.2020; 09(03): 130. CrossRef - Analysis of the Potential Association of Drug-Metabolizing Enzymes CYP2C9*3 and CYP2C19*3 Gene Variations With Type 2 Diabetes: A Case-Control Study
Imadeldin Elfaki, Rashid Mir, Faisel Mohammed Abu-Duhier, Chandan Kumar Jha, Adel Ibrahim Ahmad Al-Alawy, Abdullatif Taha Babakr, Salem Abd El-Hadi Habib
Current Drug Metabolism.2020; 21(14): 1152. CrossRef - What is the optimal time for measuring glucose concentration to detect steroid-induced hyperglycemia in patients with rheumatic diseases?
Güven Barış Cansu, Döndü Üsküdar Cansu, Bengür Taşkıran, Şule Yaşar Bilge, Muzaffer Bilgin, Cengiz Korkmaz
Clinical Biochemistry.2019; 67: 33. CrossRef - Risedronate Attenuates Podocyte Injury in Phosphate Transporter-Overexpressing Rats
Yohei Asada, Takeshi Takayanagi, Tsukasa Kawakami, Eisuke Tomatsu, Atsushi Masuda, Yasumasa Yoshino, Sahoko Sekiguchi-Ueda, Megumi Shibata, Tomihiko Ide, Hajime Niimi, Eishin Yaoita, Yusuke Seino, Yoshihisa Sugimura, Atsushi Suzuki
International Journal of Endocrinology.2019; 2019: 1. CrossRef - Novel aspects of PCSK9 and lipoprotein receptors in renal disease-related dyslipidemia
Pragyi Shrestha, Bart van de Sluis, Robin P.F. Dullaart, Jacob van den Born
Cellular Signalling.2019; 55: 53. CrossRef - Understanding the burden of refractory myasthenia gravis
Christiane Schneider-Gold, Tim Hagenacker, Nico Melzer, Tobias Ruck
Therapeutic Advances in Neurological Disorders.2019; 12: 175628641983224. CrossRef - Drug-induced diabetes type 2: In silico study involving class B GPCRs
Dorota Latek, Ewelina Rutkowska, Szymon Niewieczerzal, Judyta Cielecka-Piontek, Arun Shukla
PLOS ONE.2019; 14(1): e0208892. CrossRef - Periodically repeated rituximab administrations in children with refractory nephrotic syndrome: 2-year multicenter observational study
Toshiyuki Takahashi, Takayuki Okamoto, Yasuyuki Sato, Takeshi Yamazaki, Asako Hayashi, Hayato Aoyagi, Michihiko Ueno, Norio Kobayashi, Kimiaki Uetake, Masanori Nakanishi, Tadashi Ariga
Pediatric Nephrology.2019; 34(1): 87. CrossRef - Management of hyperglycaemia in persons with non-insulin-dependent type 2 diabetes mellitus who are started on systemic glucocorticoid therapy: a systematic review
Milos Tatalovic, Roger Lehmann, Marcus Cheetham, Albina Nowak, Edouard Battegay, Silvana K Rampini
BMJ Open.2019; 9(5): e028914. CrossRef - The effect of diabetes mellitus on in-hospital hyperglycemia, length of stay and survival in patients with brain tumor receiving dexamethasone: A descriptive and comparative analysis
Panteleimon Pantelidis, Parmenion P. Tsitsopoulos, Eleni Pappa, Elpida Theologou, Nikolaos Karanikolas, Christos Drosos, Christos Tsonidis
Clinical Neurology and Neurosurgery.2019; 184: 105450. CrossRef - Impact of glucocorticoid treatment before pregnancy on glucose homeostasis of offspring exposed to glucocorticoid in adult life
Flávia Natividade da Silva, Henver Simionato Brunetta, Maciel Alencar Bruxel, Felipe Azevedo Gomes, Alex Rafacho
Life Sciences.2019; 237: 116913. CrossRef - One week of continuous corticosterone exposure impairs hepatic metabolic flexibility, promotes islet β-cell proliferation, and reduces physical activity in male C57BL/6 J mice
Susan J. Burke, Heidi M. Batdorf, Tai-Yu Huang, Joseph W. Jackson, Katarina A. Jones, Thomas M. Martin, Kristen E. Rohli, Michael D. Karlstad, Tim E. Sparer, David H. Burk, Shawn R. Campagna, Robert C. Noland, Paul L. Soto, J. Jason Collier
The Journal of Steroid Biochemistry and Molecular Biology.2019; 195: 105468. CrossRef - Effect of preadmission glucocorticoid therapy on 30-day mortality in critically ill patients: a retrospective study of a mixed ICU population in a tertiary hospital
Tak Kyu Oh, In-Ae Song, Jae Ho Lee, Cheong Lim, Young-Tae Jeon, Hee-Joon Bae, You Hwan Jo
Annals of Intensive Care.2019;[Epub] CrossRef - Hospitalization as an Opportunity to Optimize Glycemic Control in Oncology Patients
Amy Hiestand, James Flory, Ritika Chitkara
Current Diabetes Reports.2019;[Epub] CrossRef - Corticothérapie prolongée chez une personne âgée et diabète
J.L. Schlienger
Médecine des Maladies Métaboliques.2018; 12(7): 599. CrossRef - Activation of nuclear receptor PXR impairs glucose tolerance and dysregulates GLUT2 expression and subcellular localization in liver
Fatemeh Hassani-Nezhad-Gashti, Jaana Rysä, Outi Kummu, Juha Näpänkangas, Marcin Buler, Mikko Karpale, Janne Hukkanen, Jukka Hakkola
Biochemical Pharmacology.2018; 148: 253. CrossRef - Diabetes Mellitus Secondary to Cushing’s Disease
Mattia Barbot, Filippo Ceccato, Carla Scaroni
Frontiers in Endocrinology.2018;[Epub] CrossRef - MANAGEMENT OF ENDOCRINE DISEASE: Critical review of the evidence underlying management of glucocorticoid-induced hyperglycaemia
Anjana Radhakutty, Morton G Burt
European Journal of Endocrinology.2018; 179(4): R207. CrossRef - Use of parenteral glucocorticoids and the risk of new onset type 2 diabetes mellitus: A case-control study
Ala Keyany, Johannes T.H. Nielen, Patrick C. Souverein, Frank de Vries, Bart van den Bemt
Diabetes Research and Clinical Practice.2018; 139: 100. CrossRef - Dominance of the hypothalamus-pituitary-adrenal axis over the renin-angiotensin-aldosterone system is a risk factor for decreased insulin secretion
Makoto Daimon, Aya Kamba, Hiroshi Murakami, Satoru Mizushiri, Sho Osonoi, Kota Matsuki, Eri Sato, Jutaro Tanabe, Shinobu Takayasu, Yuki Matsuhashi, Miyuki Yanagimachi, Ken Terui, Kazunori Kageyama, Itoyo Tokuda, Shizuka Kurauchi, Shigeyuki Nakaji
Scientific Reports.2017;[Epub] CrossRef
- COVID‐19 associated mucormycosis surge: A review on multi‐pathway mechanisms

- Clinical Study
- Glucose-Dependent Insulinotropic Peptide Level Is Associated with the Development of Type 2 Diabetes Mellitus
- Sunghwan Suh, Mi Yeon Kim, Soo Kyoung Kim, Kyu Yeon Hur, Mi Kyoung Park, Duk Kyu Kim, Nam H. Cho, Moon-Kyu Lee
- Endocrinol Metab. 2016;31(1):134-141. Published online March 16, 2016
- DOI: https://doi.org/10.3803/EnM.2016.31.1.134
- 3,819 View
- 44 Download
- 7 Web of Science
- 6 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader Background Incretin hormone levels as a predictor of type 2 diabetes mellitus have not been fully investigated. Therefore, we measured incretin hormone levels to examine the relationship between circulating incretin hormones, diabetes, and future diabetes development in this study.
Methods A nested case-control study was conducted in a Korean cohort. The study included the following two groups: the control group (
n =149), the incident diabetes group (n =65). Fasting total glucagon-like peptide-1 (GLP-1) and total glucose-dependent insulinotropic peptide (GIP) levels were measured and compared between these groups.Results Fasting total GIP levels were higher in the incident diabetes group than in the control group (32.64±22.68 pmol/L vs. 25.54±18.37 pmol/L,
P =0.034). There was no statistically significant difference in fasting total GLP-1 levels between groups (1.14±1.43 pmol/L vs. 1.39±2.13 pmol/L,P =0.199). In multivariate analysis, fasting total GIP levels were associated with an increased risk of diabetes (odds ratio, 1.005;P =0.012) independent of other risk factors.Conclusion Fasting total GIP levels may be a risk factor for the development of type 2 diabetes mellitus. This association persisted even after adjusting for other metabolic parameters such as elevated fasting glucose, hemoglobin A1c, and obesity in the pre-diabetic period.
-
Citations
Citations to this article as recorded by- Mendelian randomization analyses suggest a causal role for circulating GIP and IL-1RA levels in homeostatic model assessment-derived measures of β-cell function and insulin sensitivity in Africans without type 2 diabetes
Karlijn A. C. Meeks, Amy R. Bentley, Themistocles L. Assimes, Nora Franceschini, Adebowale A. Adeyemo, Charles N. Rotimi, Ayo P. Doumatey
Genome Medicine.2023;[Epub] CrossRef - Glucose- and Bile Acid-Stimulated Secretion of Gut Hormones in the Isolated Perfused Intestine Is Not Impaired in Diet-Induced Obese Mice
Jenna E. Hunt, Jens J. Holst, Sara L. Jepsen
Frontiers in Endocrinology.2022;[Epub] CrossRef - Combined treatment with a gastric inhibitory polypeptide receptor antagonist and a peptidyl peptidase-4 inhibitor improves metabolic abnormalities in diabetic mice
Fei Yang, Shan Dang, Hongjun LV, Bingyin Shi
Journal of International Medical Research.2021; 49(1): 030006052098566. CrossRef - Elevated levels of fasting serum GIP may be protective factors for diabetic retinopathy in type 2 diabetes mellitus
LingHong Huang, JingXiong Zhou, Bo Liang, HuiBin Huang, LiangYi Li
International Journal of Diabetes in Developing Countries.2021; 41(4): 543. CrossRef - Enteroendocrine K and L cells in healthy and type 2 diabetic individuals
Tina Jorsal, Nicolai A. Rhee, Jens Pedersen, Camilla D. Wahlgren, Brynjulf Mortensen, Sara L. Jepsen, Jacob Jelsing, Louise S. Dalbøge, Peter Vilmann, Hazem Hassan, Jakob W. Hendel, Steen S. Poulsen, Jens J. Holst, Tina Vilsbøll, Filip K. Knop
Diabetologia.2018; 61(2): 284. CrossRef - Articles inEndocrinology and Metabolismin 2016
Won-Young Lee
Endocrinology and Metabolism.2017; 32(1): 62. CrossRef
- Mendelian randomization analyses suggest a causal role for circulating GIP and IL-1RA levels in homeostatic model assessment-derived measures of β-cell function and insulin sensitivity in Africans without type 2 diabetes

- Obesity and Metabolism
- Sex Factors in the Metabolic Syndrome as a Predictor of Cardiovascular Disease
- Sunghwan Suh, Jongha Baek, Ji Cheol Bae, Kyoung-Nyoun Kim, Mi Kyoung Park, Duk Kyu Kim, Nam H. Cho, Moon-Kyu Lee
- Endocrinol Metab. 2014;29(4):522-529. Published online December 29, 2014
- DOI: https://doi.org/10.3803/EnM.2014.29.4.522
- 4,681 View
- 37 Download
- 16 Web of Science
- 17 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader Background Metabolic syndrome (MetS) is a condition characterized by a cluster of metabolic disorders and is associated with increased risk of cardiovascular disease (CVD). This study analyzed data from the Korean Health and Genome Study to examine the impact of MetS on CVD.
Methods A total of 8,898 subjects (4,241 males and 4,657 females), 40 to 69 years of age, were enrolled and evaluated for the development of new onset CVD from 2001 to 2012 (median 8.1 years of follow-up).
Results The prevalence of MetS at baseline was 22.0% (932/4,241) and 29.7% (1,383/4,657) in males and females, respectively. MetS was associated with increased risk of coronary heart disease (CHD; hazard ratio [HR], 1.818; 95% confidence interval [CI], 1.312 to 2.520 in males; HR, 1.789; 95% CI, 1.332 to 2.404 in females) and CVD (HR, 1.689; 95% CI, 1.295 to 2.204 in males; HR, 1.686; 95% CI, 1.007 to 2.192 in females). Specifically, MetS was associated with risk of future stroke in females only (HR, 1.486; 95% CI, 1.007 to 2.192). Among MetS components, abdominal obesity and hypertension were independent predictors of both CHD and CVD. In addition, a higher number of MetS components correlated with higher CVD risk.
Conclusion MetS is a significant risk factor for the development of CVD although its impact varies between sexes.
-
Citations
Citations to this article as recorded by- Cardiovascular age of workers with different employment categories
Byung-Kook Lee, Jaeouk Ahn, Nam-Soo Kim, Jungsun Park, Yangho Kim
Archives of Environmental & Occupational Health.2022; 77(3): 243. CrossRef - Effects of Anthocyanin-rich Berries on the Risk of Metabolic Syndrome: A Systematic Review and Meta-analysis
Mikkel Roulund Wilken, Max Norman Tandrup Lambert, Christine Bodelund Christensen, Per Bendix Jeppesen
Review of Diabetic Studies.2022; 18(1): 42. CrossRef - Rate and risk factors of metabolic components and component combinations according to hypertension status in Tibetans in a cross-sectional study
Jihong Hu, Brian Thompson, Shuxia Wang, Minhao Guo, Chunjuan Yan, Fengfeng Ding, Peng Guo, Li Chen, Zhuoma Cao, Jianzong Wang
Medicine.2022; 101(43): e31320. CrossRef - Gender differences in changes in metabolic syndrome status and its components and risk of cardiovascular disease: a longitudinal cohort study
Azra Ramezankhani, Fereidoun Azizi, Farzad Hadaegh
Cardiovascular Diabetology.2022;[Epub] CrossRef - The Association of Metabolic Syndrome with the development of cardiovascular disease among Kazakhs in remote rural areas of Xinjiang, China: a cohort study
Wenwen Yang, Shuxia Guo, Haixia Wang, Yu Li, Xianghui Zhang, Yunhua Hu, Heng Guo, Kui Wang, Yizhong Yan, Jingyu Zhang, Jiaolong Ma, Lei Mao, Lati Mu, Jiaming Liu, Yanpeng Song, Changjing Li, Zhuo Ma, Rulin Ma, Jia He
BMC Public Health.2021;[Epub] CrossRef - Serum Arylsulfatase and Acid Phosphatase Activity in Patients with Metabolic Syndrome as a Result of Oxidative Damage to Lysosomes
Dorota M. Olszewska-Słonina
Protein & Peptide Letters.2021; 28(11): 1246. CrossRef - Validation of Risk Prediction Models for Atherosclerotic Cardiovascular Disease in a Prospective Korean Community-Based Cohort
Jae Hyun Bae, Min Kyong Moon, Sohee Oh, Bo Kyung Koo, Nam Han Cho, Moon-Kyu Lee
Diabetes & Metabolism Journal.2020; 44(3): 458. CrossRef - The Prevalence of Obesity and Metabolic Syndrome in the Korean Military Compared with the General Population
Jung Hwan Lee, Da Hea Seo, Min Jung Nam, Geon Hui Lee, Dong Hee Yang, Min Joo Lee, Ung-Rim Choi, Seongbin Hong
Journal of Korean Medical Science.2018;[Epub] CrossRef - Relationship between serum bilirubin levels and cardiovascular disease
Sunghwan Suh, Young Rak Cho, Mi Kyoung Park, Duk Kyu Kim, Nam H. Cho, Moon-Kyu Lee, Christian Herder
PLOS ONE.2018; 13(2): e0193041. CrossRef - Comparison Between Metabolic Syndrome and the Framingham Risk Score as Predictors of Cardiovascular Diseases Among Kazakhs in Xinjiang
Wenwen Yang, Rulin Ma, Xianghui Zhang, Heng Guo, Jia He, Lei Mao, Lati Mu, Yunhua Hu, Yizhong Yan, Jiaming Liu, Jiaolong Ma, Shugang Li, Yusong Ding, Mei Zhang, Jingyu Zhang, Shuxia Guo
Scientific Reports.2018;[Epub] CrossRef - Impact of interactions among metabolic syndrome components on the development of cardiovascular disease among Kazakhs in Xinjiang
Wenwen Yang, Xiang Gao, Xianghui Zhang, Yunhua Hu, Heng Guo, Kui Wang, Yizhong Yan, Jia He, Jingyu Zhang, Jiaolong Ma, Lei Mao, Lati Mu, Jiaming Liu, Shugang Li, Yusong Ding, Mei Zhang, Rulin Ma, Shuxia Guo, Mahesh Narayan
PLOS ONE.2018; 13(10): e0205703. CrossRef - Prediction of cardiovascular disease in Korean population: based on health risk appraisal of national health screening program
Jae Moon Yun, Tae Gon Yoo, Seung-Won Oh, Be Long Cho, Eunyoung Kim, Insob Hwang
Journal of the Korean Medical Association.2017; 60(9): 746. CrossRef - Metabolic Syndrome Is a Strong Risk Factor for Minor Ischemic Stroke and Subsequent Vascular Events
Guang-Sheng Wang, Dao-Ming Tong, Xiao-Dong Chen, Tong-Hui Yang, Ye-Ting Zhou, Xiao-Bo Ma, Gianpaolo Reboldi
PLOS ONE.2016; 11(8): e0156243. CrossRef - Metabolic syndrome related to cardiovascular events in a 10-year prospective study
Laura Kazlauskienė, Jūratė Butnorienė, Antanas Norkus
Diabetology & Metabolic Syndrome.2015;[Epub] CrossRef - Articles in 'Endocrinology and Metabolism' in 2014
Won-Young Lee
Endocrinology and Metabolism.2015; 30(1): 47. CrossRef - Impact of Cadmium Exposure on the Association between Lipopolysaccharide and Metabolic Syndrome
Seung Han, Kyoung Ha, Ja Jeon, Hae Kim, Kwan Lee, Dae Kim
International Journal of Environmental Research and Public Health.2015; 12(9): 11396. CrossRef - Heat Killed Lactobacillus reuteri GMNL-263 Reduces Fibrosis Effects on the Liver and Heart in High Fat Diet-Hamsters via TGF-β Suppression
Wei-Jen Ting, Wei-Wen Kuo, Dennis Hsieh, Yu-Lan Yeh, Cecilia-Hsuan Day, Ya-Hui Chen, Ray-Jade Chen, Viswanadha Padma, Yi-Hsing Chen, Chih-Yang Huang
International Journal of Molecular Sciences.2015; 16(10): 25881. CrossRef
- Cardiovascular age of workers with different employment categories

- A Case of Graves' Disease Presented as Generalized Seizure Attack.
- So Young Park, Su Kyoung Park, Sung Hwan Suh, Duk Kyu Kim, Sang Ho Kim, Mi Kyoung Park, Song Yee Han, Seung Hee Ryu, Su Mi Woo, Sung Woo Lee, Neul Bom Yoon
- Endocrinol Metab. 2012;27(2):142-146. Published online June 20, 2012
- DOI: https://doi.org/10.3803/EnM.2012.27.2.142
- 23,540 View
- 34 Download
-
 Abstract
Abstract
 PDF
PDF - Hyperthyroidism is diagnosed when a patient is presented with typical symptoms, such as weight loss, palpitation, and hand tremor. However, early diagnosis is difficult in elders, because they have no typical symptoms, but only cardiovascular or muscular symptoms. In hyperthyroidism, there are often with neurologic changes, leading to various neurologic symptoms. Generalized or focal seizures are rarely reported in thyrotoxicosis and thyrotoxic crisis. Further, cases of hyperthyroidism presented as generalized seizure attack are extremely rare. We report a case of hyperthyroidism. A patient is presented at the hospital with mental change, as well as generalized seizure, who was finally diagnosed to have Graves' disease. A 56-year-old male was admitted to the hospital because of mental change with generalized seizure attack. Initial neurologic evaluations, including a brain magnetic resonance imaging and electroencephalogram proved to be normal. But, thyroid function test showed abnormal results. We diagnosed him as Graves' disease and prescribed anti-thyroid drug. Thereafter, there has been no recurrence of neurologic symptoms for 12 months.

- A Case of Primary Hyperparathyroidism with Rapid Regression of a Brown Tumor after Parathyroidectomy.
- Ji Young Mok, Ha Yeon Kim, Hsing Chien Ter, Sang Ock Kim, Dong Kyun Kim, Ji Sun Han, So Young Park, Sa Rah Lee, Mi Kyoung Park, Duk Kyu Kim
- J Korean Endocr Soc. 2010;25(1):50-55. Published online March 1, 2010
- DOI: https://doi.org/10.3803/jkes.2010.25.1.50
- 1,803 View
- 30 Download
-
 Abstract
Abstract
 PDF
PDF - Primary hyperparathyroidism is mainly caused by parathyroid adenoma (85%) and is characterized by hypercalcemia, osteoporosis, renal stones, and gastrointestinal and neurological disorders. Because of improvements in blood analysis over the last two decades, primary hyperparathyroidism is typically diagnosed early and asymptomatically. A rare clinical manifestations of primary hyperparathyroidism, brown tumors (osteitis fibrosa cystica), are osteolytic lesions resulting from long-term hyperparathyroidism. Radiologically, it is difficult to distinguish a brown tumor from plasmacytoma, multiple myeloma, or bone metastasis. We report a case of a 44-year-old man with primary hyperparathyroidism that caused a large brown tumor (11 x 5 x 8 cm) that mimicked plasmacytoma or cancer metastasis on pelvic magnetic resonance imaging. After a bone biopsy report that was highly suggestive of a brown tumor, serum calcium and intact parathyroid hormone levels were determined. The lesion was ultimately diagnosed as a brown tumor and a parathyroidectomy was performed. After 1 year, the lesion has nearly regressed by follow up of the anteroposterior view of the pelvis and bone mineral density has improved. The present case highlights the importance of considering brown tumors in the evaluation of patients presenting with hypercalcemia and osteolytic lesions without definite primary neoplasm.

- The Effect of Fenofibrate and Exercise on Metabolic Syndrome and Hepatic Steatosis in OLETF Rats.
- Kyung II Lee, Ji Min Kim, Ja Young Park, Ja Won Kim, Ji Young Mok, Mi Kyoung Park, Hye Jeong Lee, Sook Hee Hong, Wenjun Li, Duk Kyu Kim
- J Korean Endocr Soc. 2007;22(3):192-202. Published online June 1, 2007
- DOI: https://doi.org/10.3803/jkes.2007.22.3.192
- 2,129 View
- 22 Download
- 1 Crossref
-
 Abstract
Abstract
 PDF
PDF - BACKGROUND
The aim of this study is to verify the effects of fenofibrate monotherapy and fenofibrate combined with exercise for improving metabolic syndrome and hepatic steatosis. METHODS: Thirty-four weeks old OLETF rats (Otsuka Long-Evans Tokushima Fatty Rats, n = 20) were divided four groups: the regular diet group (n = 5, DD group), the exercise group (n = 5, DE group), the fenofibrate (100 mg/kg) treated group (n = 5, DF group) and the combination treatment group {fenofibrate and exercise (n = 5, EF group)}. After 5 weeks of treatment, blood was drawn for measuring the blood glucose, insulin, lipid and leptin levels. All the subjects were sacrificed for assessment of their body adiposity and hepatic steatosis. RESULTS: The total amount of food intake, body weight and total body weight of the rat were significantly decreased in the EF and DF groups compared to the DD group. The plasma triglyceride and glucose levels were significantly decreased in the EF and DF groups compared to the DD group. The HOMA-IR of EF, DF and DE groups were significantly decreased compared with that of the DD group. The plasma leptin levels of the EF and DF groups were significantly decreased compared with those of the DD and DE groups. The hepatic steatosis index was significantly decreased in the EF and DF groups compared to the DD and DE groups. CONCLUSION: Fenofibrate monotherapy was effective to control three major components (obesity, hypertriglyceridemia and hyperglycemia) of metabolic syndrome and hepatic steatosis in OLETF rats. Exercise combined with fenofibrate treatment showed an additional effect compared to that of fenofibrate monotherapy. -
Citations
Citations to this article as recorded by- Effect of Fenofibrate and Exercise on Metabolic Syndrome and Hepatic Steatosis
Bong Soo Cha, Jae Hyuk Lee
Journal of Korean Endocrine Society.2007; 22(3): 188. CrossRef
- Effect of Fenofibrate and Exercise on Metabolic Syndrome and Hepatic Steatosis


 KES
KES

 First
First Prev
Prev



